Definition – Symptoms – Causes – Tests – Treatments – Advancements
Gastroparesis:
Just Imagine…
Can you imagine never being able to eat again? Hooking up to IV nutrition or tube feedings every day in order to live? Carrying your nutrition on your back all day or being attached to a pole all night? Or, simply having to “survive” on chicken broth, Ensure, and small bites of food all day long? And in spite of that, still dealing with malnutrition, dehydration, weight loss, abdominal pain, nausea, and vomiting on a daily basis?
Frequent trips to the ER and hospital become routine…just a part of life. Social activities are non-existent because most of them involve food. If you do go out, you end up ordering water, maybe a soda, and pulling that pack of crackers out of your purse to nibble at. You feel fortunate that you are even capable of keeping that down, realizing that many people in similar situations can’t. Making plans is a challenge. You may feel well and up for an outing, but then while out the symptoms attack and a planned fun-filled evening becomes a drag very quickly. That’s what life with gastroparesis and intestinal pseudo-obstruction is like.
These conditions are so poorly understood. They are so hidden that people often don’t believe they are real or are not as serious as they actually are. Although difficult to understand, patients suffering from GP and CIP may look completely healthy. They may drive, work, shop, go to church, take care of a family, and look great on the outside. Their color may be nice, they may look strong and energetic, and they may appear to be feeling well. Yet, the turmoil churning within them is by no means normal.
Remember the last time you had the flu. After 24 hours of nausea, vomiting, perhaps diarrhea, and aches and pains, you couldn’t wait to get back to work and your normal activities. As you tried to return to your routine activities, however, you did notice you felt weaker than usual. It was more challenging to get things done because you had a day of surviving on toast, crackers, and soup…not exactly a champions dinner!
Now, take that day and multiply it by years. Add medication, medical procedures, hospitalizations, chronic malnutrition complications, invasive treatments, surgeries, and additional illnesses that develop over time. You are getting closer to understanding what life with GP and CIP is like, but you are still not there.
On top of the physical issues, because the conditions are so poorly understood, people with GP and CIP often have to live with the challenges of stereotyping by society. It is often believed that patients are exaggerating their conditions because they don’t “look sick.” Others believe those who suffer really just have an eating disorder and use a “mild” condition as an excuse for not eating well. People simply don’t understand that a couple sips of soup can send one’s gut into a frenzy and result in hours of nausea, abdominal pain, and vomiting. Sometimes this lasts even for days. One wrong bite of food can result in a bowel obstruction and trip to the hospital for an NG tube for suction or surgery to remove the blockage. There are no cold and flu treatments to help symptoms or treat the conditions at all. At best, patients can try some anti-nausea medications with nasty side effects, or drugs that are so expensive insurance companies only provide 12 a month…so they have to decide which 12 times a month they are sick enough to take it. On top of that, any drugs that may help are pulled from the market and no longer available. Once that is removed, even if restarted through compassionate clearance programs, they never quite work as well again. But the odds of getting on that program are slim to none. They feel like everything has been taken away from them…not only health, a normal life, food, and even friends and family who jump ship, but the only treatment that keeps them even somewhat functioning.
Think back again to the day you had the flu. You probably did not want to lift your head off the bed or couch. You felt too weak to make it to the bathroom. Every time you sat up, you felt your head spin and the nausea increased even more. Finally, it was a battle of determination to force yourself up and walk to distance to the bathroom. While you were up, you tried to grab as many items as you needed so you didn’t have to get back up again for a long time. By the time you get back to bed, you were so weak and wiped out that all you wanted to do is sleep or watch TV. But you couldn’t get your mind off the nausea. It was so overwhelming that you curled up into a ball on your side and just waited for it to pass. You took flu medication in hopes of sleeping it off and had hope that tomorrow would be better.
People with GP and CIP don’t have that hope that tomorrow will be better right now. Each day varies and some are better than others, but inevitably the bad days will always come back. There are limited options to treat symptoms, but they don’t work well. Patients are basically told to “live with it.” In some cases, it can’t be lived with. While most people with GP get by on what is available, because there are no other options, quality of life is certainly very poor. Many survive on less than 1,000 calories a day, severe weight loss, disability, tube feedings, IV nutrition, medication with nasty side effects, and a life full of invasive medical treatments and hospitalizations. GP and CIP are not just simple illnesses which can be cured through diet changes, medication, or surgery. They do not mildly impact life. They have a profound influence on every daily activities, regardless of severity. There is no escape. Is this the kind of life a person wants to “just live with?”
There are also many situations in which living with GP and CIP are no longer an option. In severe cases, chronic malnutrition takes over and people are unable to survive the trauma on the body. The body often quits absorbing, organs shut down, and the liver may fail for those who have been on long term IV nutrition. Veins become inaccessible and there is no way for them to receive nutrition. Some who are fortunate enough to be aware of the option and be eligible may pursue a five organ transplant as a last resort to stay alive. While this can be miraculous and life saving, it doesn’t come without its own complications for life. Individuals who reach this level of severity have become desperate. There are no options. They either risk their lives by going through a transplant, recognizing that even if they make it to the transplant and out of the OR, they face a lifetime of complications and possible organ rejection. But the only other option is starvation. There’s not really a choice when you get to that point.
Living with GP and CIP is hard to describe. The best patients can do to help others understand is to tell people to consider what it would feel like to have the flu, every single day, and the impact that would have on your life. But then you have to throw in additional health problems and the stereotypes, comments, and claims by others that what they deal with is not real and not worthy of attention. Because they don’t “look” sick, family and friends who don’t believe put a wedge between them or completely leave, believing that the person is trying to use a mild condition to “benefit” from resources such as disability, have an excuse to get out of unwanted duties, a way to receive special parking “privileges,” and other accommodations at work and school. They are often looked at oddly when forced to admit they are on disability because of a “stomach” problem, can’t lift a box of sodas into their cars because they are too weak, get glared at because they park in an HP spot but get out of the car walking, and dealing with other colleagues and students who are jealous of the accommodations received to make life easier to live and adaptation into society easier.
GP and CIP need more attention. People don’t understand what it is really like to fight these conditions and what daily life is like for those who suffer. They are downplayed as simply being conditions that can be controlled if “you would just eat correctly and avoid certain foods.” While in some instances this is true, there is a very wide spectrum to the level that people die from these conditions as well. If not to the point of dying physically, many are unable to truly “live” at all as GP and CIP zaps the life out of them. Note how long it took you to recover from just a 24 hour flu. Then realize that in GP and CIP there is no recovery. There is no in between. It is a daily battle, with ups and downs, unknowns, and a life full of complexity and misunderstanding. Try to step into their shoes for a short time. Next time you have your head in the toilet, imagine life like that every day. Be thankful for what you have. Be thankful you will recover and life will return to normal. And remember those whose lives will never return to normal. Give back. Help them fight. Support them. Try to understand. Let them vent without judging them. Encourage them. They often lack self-confidence because they have either been judged so much or feel as if they are incapable of accomplishing important things because of being ill. Also, realize that you are dealing with some of the strongest, toughest, people you will ever meet. Thank you for taking the time to read this and step into the lives of those suffering from GP and CIP for a short time.
From Wikipedia:
Gastroparesis, also called delayed gastric emptying, is a medical condition consisting of a paresis (partial paralysis) of the stomach, resulting in food remaining in the stomach for a longer period of time than normal. Normally, the stomach contracts to move food down into the small intestine for digestion. The vagus nerve controls these contractions. Gastroparesis may occur when the vagus nerve is damaged and the muscles of the stomach and intestines do not work normally. Food then moves slowly or stops moving through the digestive tract.
- Nausea *
- Vomiting
- Early satiety *
- GERD *
- Weight Loss *
- Burping
- Abdominal Distention *
- Malnutrition/Vitamin/Mineral Difficiencies *
- Uncontrollable Blood Sugar Levels
* Personally experienced
Causes of gastroparesis vary between each individual patient just as the symptoms vary. However, it is hypothesized that damage to the main nerve controlling stomach function (vagus nerve) causes most cases of gastroparesis. Damage can be from the common virus, abdominal surgery and diabetes. Sometimes the cause of gastroparesis is never determined and this is called idiopathic gastroparesis.
Diagnosing gastroparesis is often a matter of elimination. This is because it doesn’t always show up in tests. There are ways to directly diagnose it, but they are by no means a way to prove someone isn’t suffering from gastroparesis. Common diagnostic tests include but are not limited to:
- Medical history of symptoms
- A nuclear medical test called a gastric emptying study, the golden standard for diagnosing gastroparesis.
- Upper GI endoscopy
- Antro-duodenal motility study
- X-rays and CT scans
* My personal experience with all types of treatments can be found here.
Because the cause of gastroparesis is often unidentified, treatment aims more at controlling symptoms, rather than curing the problem. Treatments come in all forms such as diet changes/restrictions, medications, enteral nutrition and even surgery in the most severe cases.
Diet changes are often made based on the fact that the stomach is slow or non-functioning. Anything taken by mouth that would further slow down digestion is to be avoided. Foods high in fiber or fat will slow down the stomach. Vegetables, red meat, fried or fatty foods are all on the list of foods to avoid when you suffer from gastroparesis. Same goes for anything fortified with fiber. I find that staying away from any artificial sweeteners is also beneficial.
When diagnosed with gastroparesis and a change in diet is your first step of treatment, it is important to consult with a dietician or nutritionist to make sure your body is receiving what it needs. They can also help develop meal plans in oder to eliminate the foods that may cause more intestinal distress due to gastroparesis. Everyone is different. What foods work for one individual, may not necessarily work for another. This process is often slow but necessary so you don’t continually make yourself sick by eating the wrong food for your body. For more information on GP diet guides, visit GPDA’s Gastroparesis Diet.
When diet modification isn’t enough to control the symptoms of gastroparesis, medication is often the next step in treatment. Medications aim at increasing motility of the digestive system, especially the stomach. These medications include:
- Erythromycin (Benzamycin)
- Metoclopramide (Reglan)
- Domperidone
* My medication experience and list of maintenance medications
If medications are not effective enough, the other options such as tube feeding and surgery for a gastric neurostimulator should be investigated. These are usually last resort options. Medications and diet modification is usually enough to control symptoms.
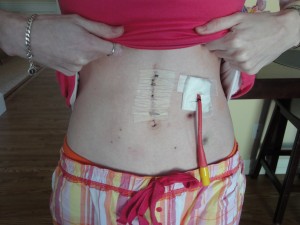
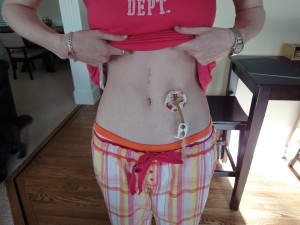
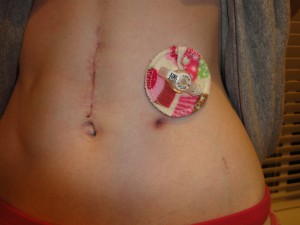
Tube feeding is generally directed straight into the upper part of the intestine called the jejunum. It bypasses the malfunctioning stomach and is able to deliver nutrition. There are many different types of tubes from nasojejunal tubes (usually temporary to determine if you are able to handle tube feeds and is often placed endoscopically, under sedation by your GI or radiology), surgical tubes, endoscopically placed tubes (PEJ), and low profile tubes. Low profile feeding tubes are generally placed only after the stoma site has fully healed from a PEJ. It is important that the tract between the stoma and intestine be fully formed before a button is placed. If that tract breaks down during the procedure, you might experience complications like me. Your doctor can discuss with you, the best tube for your situation. I have had all four types of tubes as seen below.
* My tubes experience
The final stage in treatment is surgery. The current type of surgery performed is implantation of a gastric neurostimulator. A gastric neurostimulator, or stomach pacemaker, helps control nausea and vomiting by electrically stimulating nerves in the stomach. For some patients, the relief is instant while others take up to a year to notice any difference. It is not approved for improving gastric emptying but many hope that with time, they will notice a difference in that as well.
The surgery for a neurostimulator is typically between 1 and 2 hours with a hospital stay of 2-3 days. Pain from the procedure is like any other open surgery. For me, pain was easily controlled through IV medication and at home with oral medication. I required only a week or so for recovery before I felt well enough to get out and do things. The device can be remotely accessed in your doctor’s office after the procedure. Adjustments are made individually and many adjustments are usually needed to fully take advantage of the device.
* My surgery experience
There are positive advancements being made in the treatment of gastroparesis.
Tranzyme
Also known as Ulimorelin, this drug Tranzyme Pharma (TZP) has shown extremely positive results in controlled testing of diabetic gastroparesis. It has shown to be a potent prokinetic drug, significantly reducing nausea and vomiting while promoting gastric emptying. The furthest testing phase is seen with the IV delivered drug (TZP-101) but the oral (TZP-102) trials are not far behind. If this drug does what studies show it to be doing, it would be a very exciting bit of information for so many of us plagued by the disease of gastroparesis (idiopathic or otherwise) and the symptoms it produces.
To follow the progression of the developing treatments of TZP, visit:
- Tranzyme Pharma’s Clinical Results on Ulimorelin
- Tranzyme Pharma Press Release (June 29, 2010)
- Positive reports from TZP102 and diabetic gastroparesis
* For more information centering around gastroparesis, feel free to visit my Recipes page, Spoon Theory page and Open Letter *
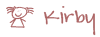







55 Responses
Beth says...
I have recently been diagnosed with GP after about 15 years of stomach issues. I was actually relieved to find out there was actually something wrong with me, for a while I was made to think it was all in my head! I am overweight now, but had a massive weight loss about 15 to 20 years ago. I am an emotional eater, so when I am depressed about not getting to eat normally or enjoy time with my family, it is hard to stick with the liquids. I do not want this disease to affect others around me, but I know it is. I am not sure where to go from here. I am now taking Reglan, but not sure what the next step for me should be since I am not underweight, just sick of the pain! Any suggestions?
Amber says...
Thank you so much for sharing your journey. My Mom was just diagnosed with gp and is experiencing very bad side effects from the reglan. She is going through a deep depresion and is experiencing severe anxiety because of the diagnosis. Your posts have helped me understand more of the road she is facing. Thank you again.
sarah says...
I have been wondering how you are doing ….looking at getting a j tube. Did you story end well? Have heard some scarey tube stories please tell me it saved your life and are doing great.
Mary Ann says...
I find it fascinating that after all of these years, there is finally a name to this horrible chronic and life altering illness. My onset of the illness was when I was 13. At the time doctors didn’t know how to treat the case and as I grew weaker and weaker, they transferred me to the arnold pamler childrens hospital, where i was placed with a PICC line in order to get lipoproteins and TPN into the body. After traveling all over the east coast, doctors at John Hopkins studied my case and determined it “Gastro-duodenal-dysmotility-syndrome. Aka a higher degree of Gastroparesis. For the next 10yrs I lived off of TPN, lipoproteins, and a couple other supplemental ivs. Although I was able to eat, I would immediately throw up the food. Eventually i was able to balance my level of wnergy w the food id take in and theow up. my body was able to evolve in a way that acid disnt form in the system. so not only nutrients stay in the atomach longer, but when they did vomit back up, my teeth werent deatroyed.Roughly at this point in my life, after 20yrs of living w this disease, I would estimate that due to this illness I have thrown up every meal everyday (sometimes 2 or 3 more given the nausea) to roughly say: over 43,000 times. How my mutant body is still alive after all this is beyond me. But I have survived without a PICC or port or an feeding tube for the last 15yrs
Tilly says...
My 9 year old was diagnosed with gastroparesis two years ago. He’s thin and small, only 42 pounds. He has troubles eating fatty foods like meats and often carbs and cereals trigger a lot of pain. Does anyone know of some low fat foods that pack a little more calories than fruits? This kid needs to eat something with calories that doesn’t make him double over in pain!
Joe McG. says...
Thanks for saying it in a way that easy to understand. This is the worst thing I’ve ever dealt with. I’m 42, a healthy type one diabetic, who ran a marathon in November of 2010. I switched jobs in 2011 and have always had trouble with GI distress when deign with stress. It wasnt until the third ER visit that I said something is wrong. Sadly it took until the seventh trip in eight months for them to do the gastric emptying study. From April 2012 to April 2013 I lost 48lbs. Dropping from 178lbs to 130!!! I now weigh less than I did in eighth grade. I describe this disease as being in a dark room and getting punched in the face and you know you’re going to get punched again but will it be in the second round of the fight or eighth or the fifth or the eleventh
Joe McG. says...
It has basically ended my life. I feel like I’m not a man and I’ve nicknamed mysf the king of disappointment, because I’m the reason our plans always change. I don’t go on vacation with my famiky I didn’t take my son to drop him off at college and honestly I wish God would put me out of my misery. My wife is so stressed and it kills me to see it in her face. I adore this woman and I can’t do anything. We have become sick person and care taker rather than husband and wife, there’s no intimacy in our lives and I fear she will accidently find it In The form of another man. I cannot sleep I wake daily by three and seem to feel best until noon. By the time she gets home I’m sick. I’m depressed, I’m angry, I’m lost…….. I need HELP.
Elisha Weide says...
Finding your blog gave me so much hope.
I have had gastroparesis since 2011 and it has
Severely complicated my life. I’ve lost
Jobs because of it and not many seem to
understand. I do not have a feeding tube
but I still get sick most days. My energy is
constantly lower than others. I hope that some
Of your recipes can help out and that showing
Your blog to others will help them better
Understand where I’m coming from. Thank you so much.
-Elisha
Pat says...
Hi Kirby,
I tried to send an e-mail message to you, but couldn’t get it to work. So, I’m sending this via the comment section.
First, I want to say thank you: Thank you for sharing your personal experiences with Gastroparesis & CIP and the process you went thru for treatment, as well as bringing more awareness to these types of motility disorders. I have been following your blog and respective Facebook page. I came across your blog during my search for additional information and experiences; plus, my Nutritionist/Dietitian told me about your blog as well (imagine that). I have encountered other types of info, but none that approach it from a more personal viewpoint and specifically in regards to treatment modalities.
Despite what you go thru yourself, you seem very strong and resilient. That gives me hope and comfort. You are such an inspiration for me, as well as a blessing to and for me, and judging by other comments on here (thru-out all the pages), to others as well who follow your blog. So, I wanted to thank you for sharing some of your journey and letting others follow you and see a little into your world/life living with Gastroparesis and GI motility issues, along with many of the associated problems/issues & treatments that go along with it all. I know from personal experience, it’s not easy living with GI problems.
Anyway, I wanted to let you know how much your blog has touched my heart and, by sharing your experiences, how helpful your blog has been to me and I’m sure many others as well, who also follow you. You are a God-send to many. So, I wanted to tell you this first off.
My second reason for writing is I wanted to ask if you would be willing to be in communication with me. As I read your blog, we seem to have some similarities. There are very few people I feel I can related to w/in my situation. Would you be willing to communicate via e-mail (as you’re able to, of course)? Or, just whatever you feel comfortable with. The other thing that intrigued me from reading your blog is the possibility of Mito as the underlying cause of your GP/CIP, which interests me as well.
Just a little about me: I have Gastroparesis, GI Dysmotility and an overall slowing down of my gut. The Gastroparesis…I have been diagnosed for 10+ years now, was diagnosed back in 2003 after testing confirmed it, but I believe I had it for much longer than that, as I had been experiencing a lot of GI symptoms/problems for at least 5 to 6 years prior to being officially diagnosed (since 1997/98). We just never knew the reason why, until I got referred to a Gastroenterologist who happened to be familiar with motility disorders. I have a complicated history of GI problems, of which the Gastroparesis is just a part of it. I also deal with GI motility issues that extend beyond & involve more than just my stomach it seems; this includes the GI Dysmotility & the overall slow gut – not an official diagnosis yet, but we do know that my motility issues involve more than or go beyond just my stomach, and given my history we also know that it affects my intestines, just nothing specific. I am not sure if it’s an extension or progression of the GP, or a separate thing going on entirely, in addition to the GP. I also have other diagnoses as well. Anyway, that’s a little bit about me.
I hope and pray that you are staying as well as possible. You will remain in my thoughts and prayers. Thanks again for sharing your experiences. I look forward to hearing from you, and hopefully being in further communication with you, as you’re able.
Take Care & God Bless!
Pat
Toni C says...
I’ve sat here reading all of this to my parents, and it’s simply unbelievable to see how many feel exactly the same way I have for 10 years now. The feeling of being so misunderstood is no stranger to me. For years, I’ve suffered thru pain, nausea, vomiting, just all of it. I’ve had many blood transfusions, vitamin transfusion, iron transfusion, NG tubes, feeding tubes, central lines, picc lines, ports…it goes on and on. This year was the first year I had to have a shot for my bone marrow to produce red blood cells and started having seizures. A few years ago, both of my lungs were punctured multiply times by the attempt to put a central line in since I had no more veins that would support an IV. The doctor didn’t read the xrays after the process of trying to place the central line, and as I laid there dying, one nurse intervened on my behalf when she heard me saying that I could only breathe in and not out. She rushed me to the OR where I had 2 chest tubes placed, and God spared my life. I was so ready to just die to get away from this pain. EVERY day…pain. For years. I had not just grown tired, I was weary. Tired is an understatement. I ran into the same problems as some of you with doctors not wanting to relieve my pain because the narcotics would make it worse. Is that even possible to make it worse than what I was already dealing with? Well, I finally found the help I was needing at Baylor University Hospital in Dallas. My first procedure done at Baylor was the gastric stimulator. Although it did help with the nausea somewhat, it took a year to feel any measureable relief. It wasn’t until it was set all the way up to a 10 that it made a very big difference. After that, I was sent to the Pain Management division at Baylor. Thank the good Lord, on my first visit, my doctor, Dr. Toye, witnessed me in an episode of septic shock. She immediately decided that she would admit me, stabilize me and do a nerve block on my vagus nerve. I hope I spelled Vagus right. Lol She also placed me on Dilaudid, 4mg 3 times daily. FINALLY, someone saw that I could not live like I had been. She said we need to be able to help me ‘function’ again. I keyed right in on the word ‘function’. Oh, my gosh, someone gets it!, I thought. I hadn’t ‘functioned’ in years. It was such relief to have the nerve block and pain medicine together. I felt alive again, although the septic shock was still happening on a pretty regular basis. But, I wasn’t spending every single day of my life in bed at the hospital or in the bed at home, like I had for so long. The pain medicine enabled me to move around and get out some on the ‘good’ days without the effort it had taken before. The nerve blocks lasted approximately 3 months. So, in July of this year, Dr. Toye recommended we burn the nerve also to see if the relief would last longer. And, it has! Talk to your pain management team about this procedure. Now, the episodes of sepsis weren’t quite as debilitating as they had been in the past, although they certainly were no walk in the park, either. Then, my brother introduced me to a product that works better than even the strongest prescription strength laxative, Lactulose, and I’ve been able to stay out of the ER for 9 weeks straight. It’s a ‘tea’ that cleanses without dehydration, and prevents the build-up that causes us so much pain and becoming toxic, then having to have the painful NG tubes and all the other that we go through to have relief, which only usually lasts a very short time. The combination of the tea, the nerve blocks and the pain medicine, narcotic or not, has given me the longest break I’ve had out of the hospital in 2 years. I start my 9th week tomorrow. Woohoo! Thank You, Jesus! And, I go walking everyday now to try to rebuild the muscles in my legs that I’ve lost along the way. There IS hope! If anyone wants info on what products I’m using, you can email me @ mscantbwrong1119@yahoo.com. Please, never give up! I wanted to soooo many times. I just wanted to die. But, thankfully, I have renewed strength and a closer life to normal than I’ve had in 10 years this December. For, the ones just beginning this hard journey, you are not alone.