Medicine is a science of uncertainty and an art of probability. — William Osler
I apologize for not updating here, as I should, but for once I have an excuse other than pure laziness. As I mentioned briefly in the tubes section of experiences, I was approved and waiting for the outpatient procedure that would change my PEJ tube to a PEJ button. Through this procedure, I’d have a bit more freedom and experience less infections, rancid aromas and also be down one puppy chew toy. I patiently, um – as patiently as Kirby can be, waited the 2 months after original PEJ placement so that I may have my button. The button represented so many things such as the freedom previously mentioned, return to a new state of normalcy, and even a bit of beauty (no tube hanging from the body could be considered its own form of beauty).

When I got the greenlight for a button procedure, I pushed and pushed to get the procedure scheduled for the day before yesterday. I saw my doctor on Thursday (6/3/10) and was able to get an appointment for 9am the morning of June 8th. I couldn’t be more excited to finally have a date. Something solid I could work with and towards. I went out and did my hospital pajama outfit shopping routine and my OCD housecleaning. I knew I would only be gone for a day with a slight possibility of an overnight stay, but, it kept me busy – and you just never know what could happen. Well the unknown quickly became the known on the morning of the 8th in June.
I left for the hospital for a button procedure with the aid of endoscopy, at 7:45am. I was prepped and ready to go with sedatives administered at 9:30am. Even though I came in with a migraine that I had been fighting for the past few days – I knocked right out. I woke up to my husband and doctors I didn’t know. After 10 previous endoscopies, I knew this was not normal. Usually the anesthesia wears off before I see anyone and if I see any doctors, it is going to be my gastroenterologist who preforms the procedure. Confused and still groggy I was told by my husband that they were going to be rushing me in for another surgery. There were complications and the doctors were arguing back and forth about whether there would be time for ct scans and x-rays as well as pain medications like epidurals and injections (yes, it was that bad). No time for anything – into the OR I went for complications that still didn’t get explained to me. There just wasn’t time for me to fully wake up to comprehend it all.
I don’t know how long the second procedure was but I did make it out safely and with my whole intestine in tact.
[flickr-gallery mode=”tag” tags=”emergency”]
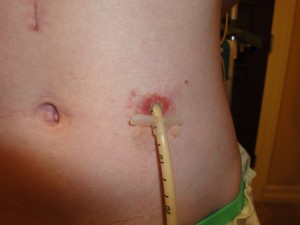
How did this all happen? What was the process? Well, to remove the original tube – they had to go through my gut endoscopically and cut off the internal bumper. Then the tube is free to be pulled out from the outside. While the first tube healed, it created almost like a vessel – a connection of tissue, if you will, between the abdominal wall and the intestine. This kept the intestine close to the wall and stable. When the first tube was removed and the new button put in, refer to this picture of the button tube, the force from pushing it through caused that tissue to break and for the intestine to pull away from the abdominal wall. This is what they meant when they kept telling me, “we lost your small intestine.”
Once the intestine was lost from view – with the hole still very much open, everything from my intestine was leaking out into my abdominal cavity quickly filling it to the point of near organ failure, with fluid, air and other types of matter. Because of the rate at which it was leaking, there was no time for CT scans, X-Rays or even an epidural, all of which the doctors were fighting to get. I was lucky not to lose my intestine during the process. During the short moments between one procedure and the next, I developed peritonitis. Another major complication to throw onto the pile. Sometime during the procedure an issue came up regarding my pacemaker. Should it stay on or off during the surgery? Cauterizers are on the no-no list of things to hang around with while having a gastric neurostimulator implanted. The doctors, again, felt there was no time to turn it off and continued with the surgery. Of course, the worst situation did happen and they cauterized right through one of the leads in my stomach. Improvising, they used some sort of electrical gel to maintain the connection and my wonderful gastroenterologist, who insisted on sitting in on the surgery, made sure it was in full working order.
I don’t know how long I was in the OR for or how long it took for me to leave the recovery room but I do know that I was back into a hospital room by 6pm. It was a very long and complicated day. I scared a lot of friends and family. I stayed in the hospital for 5 days. My stomach went from one extreme to the other:
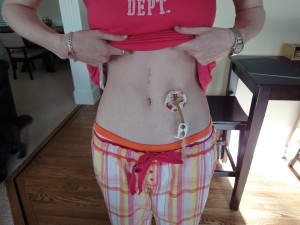
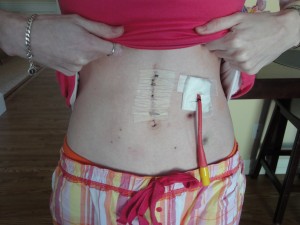
But overall, I’m doing OK. Slowly recovering and hoping to soon replace this ugly surgical tube (with no bumpers, clamp or decent plug – held in place with stitches!) with my old tube while I start the waiting game for another chance at a button. C’mon Dr. Patterson – you can do it, I know you can!